Mental Health Innovations (MHI) has provided the Shout service across the UK for the last 7 years and is still the only free, off-bill, 24/7 crisis SMS text service. In this time, we have scaled the service to support more than three million conversations with more than one million children, young people and adults who needed immediate mental health support. In response to NHS England’s Crisis Text Service Specification, we have delivered the Shout Clinical Model for over 12 months, where support is provided by mental health professionals rather than trained volunteers. The Shout Clinical Model is now contracted by 10 NHS areas across England.
Embedding a 24/7 crisis text service into local urgent care: launching Birmingham and Solihull’s partnership with Shout
Why did you choose to partner with Shout?
One of the key priorities set out in our five-year strategy for mental health is to reduce pressure on crisis services by making mental health services more accessible at an earlier stage.
With a proven track record in providing text-based mental health support at all levels of mental health need, Shout felt like a perfect fit.
Because it’s free, confidential and doesn’t show up on phone bills, our partnership with Shout removes a lot of the worries that stop people from picking up the phone. Texters aren’t just supported in the moment, they can also be signposted to local services like Talking Therapies, our Mental Health Helpline or Talking Spaces if they need more help. Knowing there’s a strong, well-established clinical framework behind the model, with clear risk and safeguarding processes, gave us real confidence this service could safely support people in all kinds of distress.
When and how did you launch?
We launched our partnership and ‘Space’ keyword in August 2025, and we made sure people heard about it. With the support of Shout, we developed a clear communications plan aiming to reach young people. In the lead up to the launch, we spent time engaging with pastoral and wellbeing leads within schools, colleges and universities – sharing a toolkit of resources created by Shout that would help them spread the word to students.
We developed a joint press release with Shout and secured a case study – a young person with lived experience who could highlight the need for our service. The launch was picked up by BBC Midlands Today, which helped us make a big impact from day one. We also received coverage in other local print and online media, as well as promoting it though pharmacies and Birmingham and Solihull Mental Health Foundation Trust’s social media and website.
Working with Shout, and their expert marketing and partnership teams, we developed and shared a toolkit of easy-to-use marketing materials with system partners so everyone could promote the new local service consistently.

What were your key successes from the launch?
One of the biggest reasons the launch landed so well was that everyone across the health and social care system in Birmingham and Solihull got behind it. Mental health teams and partner organisations shared information, used the marketing materials and signposted consistently which helped build trust quickly.
We also made sure the service featured clearly on answerphone messages for both our NHS 111 Option 2 and local Mental Health Helpline, so it immediately felt like part of the wider support network. Because we focused a lot of our outreach on young people, particularly through schools, colleges and youth-friendly social media, we saw really strong engagement from under-25s right from the start.
How have you continued to promote the service to engage texters?
We didn’t stop once the service went live. We’ve kept momentum going by promoting it everywhere young people spend time: universities, student accommodation, colleges, schools and community events.
We secured a communications budget so we could run targeted campaigns in places we knew would reach our chosen target audience. That included targeted ads on Snapchat and outdoor advertising in student and high footfall areas. Shout also promoted our keyword partnership at University Wellbeing Fairs, on local radio and led a school’s ‘Lunch and Learn’ webinar with the support of their experienced clinical team to make sure staff across the system know exactly how and where to signpost.
More recently, we’ve launched a new campaign aimed specifically at young men. They make up a smaller proportion of our texters, so in early 2026 we asked three young local men to share their stories. They featured on billboards across Birmingham - outside sporting venues and nearby local mosques - to help break stigma and encourage more men to take that first step.
In what ways has the Shout Clinical Model supported the quality and consistency of crisis support for people who may struggle to access traditional services?
The beauty of the Shout Clinical Model is that it gives people a safe, easy way to ask for help at any time of the day or night. Because it’s a text service, lots of people who may feel uncomfortable speaking out loud or need discreet support, can reach out without hesitation.
In the very first month, feedback from texters said they used the service because they wanted to talk to someone who didn’t know them, and said they simply felt more comfortable texting than talking. That tells us the model is genuinely reaching people who might otherwise stay silent.
How has the Shout Clinical Model aligned with your local NHS mental health and crisis care priorities?
Shout fits neatly into our wider vision of giving people more ways to get early help before things escalate. Our ‘Space’ keyword is available 24/7, providing early intervention and confidential listening support that sits naturally alongside other services on our urgent care pathway. Because it provides a gentle and private way to talk through difficult thoughts and emotions, many people reach out before they hit crisis point. Every conversation is handled by a qualified mental health professional, meaning texters receive real-time support grounded in strong clinical practice.
Clinicians assess risk, develop safety plans where required and follow clear safeguarding procedures. The aim is always to de-escalate early and reduce the need for more intensive crisis intervention later on. When further help is required, texters can be signposted to other services within our mental health system, or if someone is in immediate danger, emergency services are contacted to ensure prompt support.
To ensure the service works as a truly complementary part of our broader urgent care pathway, its activity data feeds into our Urgent Care Programme dashboard, helping us track trends and strengthen system oversight.
What has the first six months of delivery shown about how and when people choose to access mental health support via text compared to traditional routes?
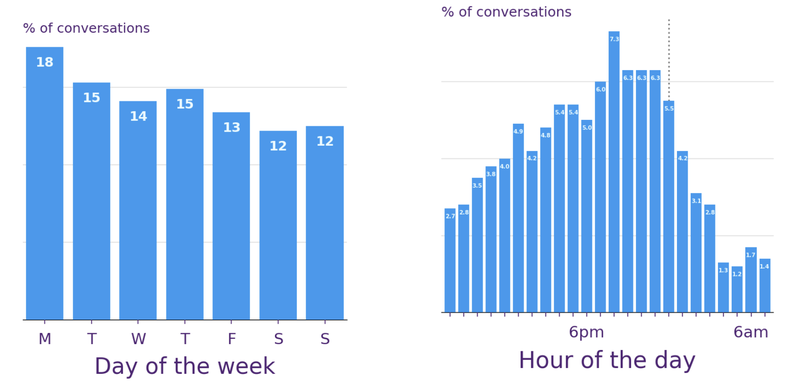
We’ve observed some patterns beginning to emerge. While activity is generally evenly spread across the week, Mondays have seen the highest level of contact. Most people text in the evenings, especially between 7pm and 11pm when other support services often aren’t available, and with a notable rise also seen at school and college finish times.
What early insights suggest the Shout service is addressing an unmet need within your local population?
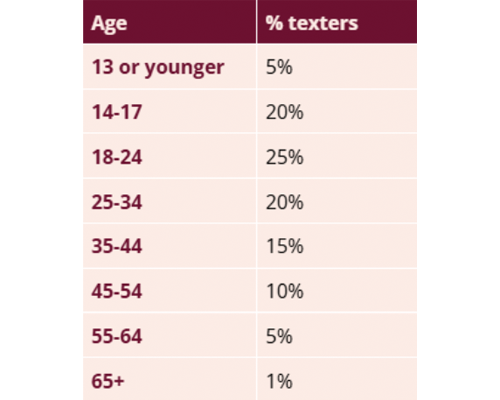
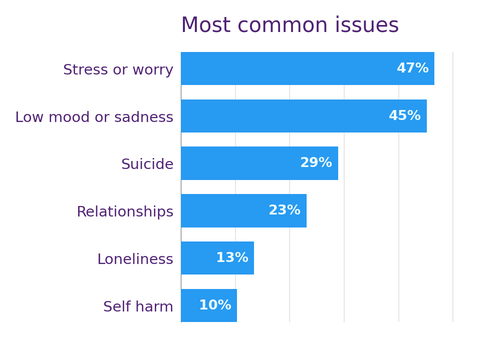
Across the first six months, hundreds of people reached out for support and new texters continue to come through each month. Young people in particular are engaging strongly, with over half of all messages coming from 14–24 year-olds. That tells us we’re filling a gap for young people who may not feel comfortable using traditional services.
The number of people accessing our ‘Space’ text service has highlighted how powerful digital support can be within an integrated mental health care system. Because texting feels low-pressure and familiar, it opens the door for conversations that might never happen otherwise.
“Working with Emma, Lyndsay and the rest of the network in Birmingham and Solihull has been a brilliant example of collaboration between the NHS and the Charity sector. We’re incredibly proud of what the Shout Clinical Model has achieved in the first six months of the partnership, showing that SMS text support has been a valuable addition to the suite of services available to the people of Birmingham and Solihull. We’re really looking forward to continuing working together and providing access to mental health support when people need it most.”
Kane Hazard
Kane Hazard, NHS Partnerships Manager at Mental Health Innovations
As set out in the Urgent and Emergency Care (UEC) Recovery Plan and the Suicide Prevention Strategy, implementing crisis SMS text services were identified as an integral step in improving access to mental health support as part of already-established care pathway.
We recently asked texters who used the national Shout service some questions to understand how they feel about accessing mental health support and who they would typically reach out to. When asked what they would do if they had not been able to text Shout, over half of respondents say they would not seek help at all without this service. Fewer than one in ten would contact NHS or emergency services directly. It is clear that the Shout service plays a critical role as an accessible first point of support and prevents many people from facing difficulties alone.
When texters to the national Shout service were asked if they had received or tried to access mental health support from NHS services in the last 12 months, 40% said they had not received or tried to access NHS mental health support, 16% were currently on a waiting list and 12% were unable to get an appointment, or did not meet the threshold for support. Only 21% were currently receiving support, and 12% had received support in the last 12 months. Demand for NHS mental health services is high, but access is constrained with more people waiting or unable to get help than are currently receiving treatment, and a large majority having never tried to access support.
We provide the Shout Clinical Model to 10 NHS regions and continue to work with our partners to help divert demand away from frontline NHS services and offer an alternative method of accessing mental health support. Alongside this, we work together to understand opportunities for integration with local crisis services as well as requirements for translation services so we can better support their communities.
Get in touch
If you would like to hear more about how the Shout Clinical Model can support people in your area, please contact kane.hazard@mhiuk.org, or complete the form below.
You might also be interested in:
-

Expanding LifeSkills: digital self-paced learning to support mental wellbeing
We're excited to launch more key topics in our LifeSkills self-paced learning modules, focused on supporting people with substance misuse and growth mindsets to help support long-term wellbeing.
-

Partner with The Mix: Supporting young people together
The Mix is the UK’s leading digital support service for young people, providing free, confidential support which can be accessed wherever young people are.
-

Shout's clinically-led service
Commissioning Shout's clinically-led service enables ICBs to deliver against NHSE advisory specifications for implementation of 24/7 crisis text message services, integrated with their local services.
